Letter to editor: Differentiating between category II pressure ulcers and herpes simplex virus skin lesions as part of skin assessments of oncology patients’ buttocks
Received:
Accepted:
Published:
Authors: Shannon Fletcher
Citation:
Fletcher S, (2026) Differentiating between category II pressure ulcers and herpes simplex virus skin lesions as part of skin assessments of oncology patients’ buttocks. Global Wound Care Journal 2 (1): 10-11.
Dear Editor
In an acute oncology hospital, between May and September 2025, the tissue viability service received 10 new referrals and incident reports for category II pressure ulcers on oncology patients’ buttocks which were in fact herpes simplex virus (HSV) skin lesions.
Pressure ulcers are defined as localised injuries to the skin and/or underlying tissue, usually over a bony prominence or medical device, resulting from sustained pressure (European Pressure Ulcer Advisory Panel [EPUAP] et al, 2019). Category II pressure ulcers are partial thickness skin loss where the top layer of skin is damaged, appearing as a shallow open sore or a blister (EPUAP et al, 2019).
HSV skin lesions can also present as blisters, vesicles or ulcers over bony prominences and could be mistaken for category II pressure ulcers [Figure 1] (Sharma et al, 2023).
Oncology patients have an increased chance of developing herpes simplex infection due to impaired cell mediated immunity (Sharma et al, 2023).
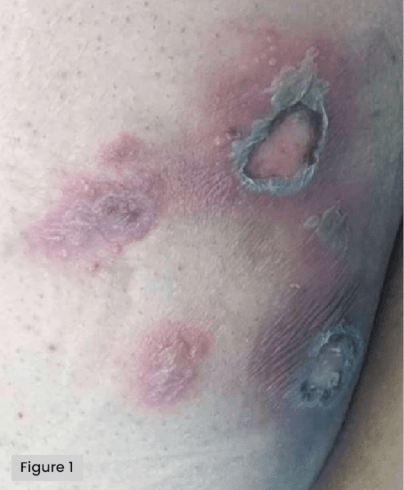
Figure 1. Herpes simplex virus skin lesions on left buttock.
Treatments of category II pressure ulcers and HSV skin lesions are individual, so need accurate diagnosis, with obtaining patient history, effective communication, thorough assessments and a good knowledge base of the assessor.
Category II pressure ulcers will only develop over a bony prominence or related to a medical device and can be painful. Patients at risk or who have active pressure injuries/ulcers should be on a care plan that addresses Assessment, Skin inspection, Surface, Keep moving (repositioning), Incontinence, Nutrition and Giving information (ASSKING bundle) for treatment and prevention of pressure ulcers (NHS Improvement, 2018).
HSV skin lesions can develop on any area of the gluteal region and have serpiginous borders (Melnychuk et al, 2024). HSV skin lesions can cause pain, itching and a tingling sensation; and may also be associated with systemic symptoms, such as fever or fatigue (Tayyar et al, 2023). Patient education is key in detecting early signs of skin changes because they may have had these lesions before and it may be a recurrence (Robijns et al, 2023).
For HSV skin lesions, aciclovir is prescribed to shorten infection duration. It is usually recommened to use 48 hours of antiviral treatment after HSV skin lesions have healed or dried, due to the possibility that immunocompromised patients may have subclinical shedding of the virus (Harfouche et al, 2025).
The national comprehensive cancer network guidelines advise HSV pharmaceutical prophylaxis with aciclovir, famciclovir or valaciclovir during active cancer therapy, with the possibility of extenstion depending on the degree of immunosuppression (Tayyar et al, 2023). Currently, there is no commercially available vaccine against HSV.
In both category II pressure ulcers and HSV lesions, good skin and wound care is essential to prevent infection or secondary bacterial infections with dressings.
In category II pressure ulcers, a silicone adhesive dressing was used to promote a moist wound healing environment, with barrier film to protect surrounding skin from moisture. Honey dressings are known to have antiviral properties, so in HSV skin lesions, a manuka honey viscose net dressing was used with a silicone adhesive dressing to secure, and barrier film to protect the surrounding skin (Rocha et al, 2022).
HSV skin lesions can be disabling, causing significant impact to the patients quality of life. Pressure ulcers also can have a profound effect, due to the poor physical condition patients experience (Roussou et al, 2023). Therefore, adequate pain relief is fundamental in both skin conditions.
If HSV skin lesions are misdiagnosed, it can delay antiviral treatments and worsen infections where lesions will coalesce and be more difficult to treat. If category II pressure ulcers are diagnosed wrongly, they increase pressure ulcer numbers for the trust. Patients will be on pressure ulcer prevention care bundles inadvertently (NHS Improvement, 2018).
In summary, healthcare professionals need to be able to differentiate between category II pressure ulcers and HSV skin lesions to be able to start the correct treatment plans. More awareness is needed that HSV lesions can occur on patients buttocks. There is also a need to look at therapeutic treatments as standard practice due to the disease burden of HSV.
References
European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel, Pan Pacific Pressure Injury Alliance (2019) Prevention and treatment of pressure ulcers/injuries: clinical practice guideline. EPUAP/NPIAP/PPPIA
Harfouche M, AlMukdad S, Alareeki A, et al (2025) Estimated global and regional incidence and prevalence of herpes simplex virus infections and genital ulcer disease in 2020: mathematical modelling analyses. Sex Transm Infect 101(4): 214–223. doi: 10.1136/sextrans-2024-056307
Melnychuk I, Gaither A (2024) Anogenital herpes simplex virus infection mimics sacral and gluteal pressure injuries. Adv Skin Wound Care 37(3):122–4. doi: 10.1097/ASW.0000000000000102
NHS Improvement (2018) Pressure ulcer core curriculum. London: NHS Improvement. Available at: https://www.england.nhs.uk/wp-content/uploads/2021/09/Pressure-ulcer-core-curriculum.pdf (accessed 07.11.2025)
Robijns J, Lodewijckx J, Claes M, et al (2023) Evaluation of a novel skin care product for the management of chemotherapy-related dermatologic toxicities: a quasi-experimental study. Eur J Oncol Nurs 63: 102278. doi: 10.1016/j.ejon.2023.102278
Rocha MP, Amorim JM, Lima WG, et al (2022) Effect of honey and propolis, compared to acyclovir, against herpes simplex virus (HSV)-induced lesions: a systematic review and meta-analysis. J Ethnopharmacol 287: 114939. doi: 10.1016/j.jep.2021.114939
Roussou E, Fasoi G, Stavropoulou A, et al (2023) Quality of life of patients with pressure ulcers: a systematic review. Med Pharm Rep 96(2): 123–30. doi: 10.15386/mpr-2531
Sharma D, Sharma S, Akojwar N, et al (2023) An insight into current treatment strategies, their limitations, and ongoing developments in vaccine technologies against herpes simplex infections. Vaccines (Basel) 11(2): 206. doi: 10.3390/vaccines11020206
Tayyar R, Ho D (2023) Herpes simplex virus and varicella zoster virus infections in cancer patients. Viruses 15(2): 439. doi: 10.3390/v15020439
